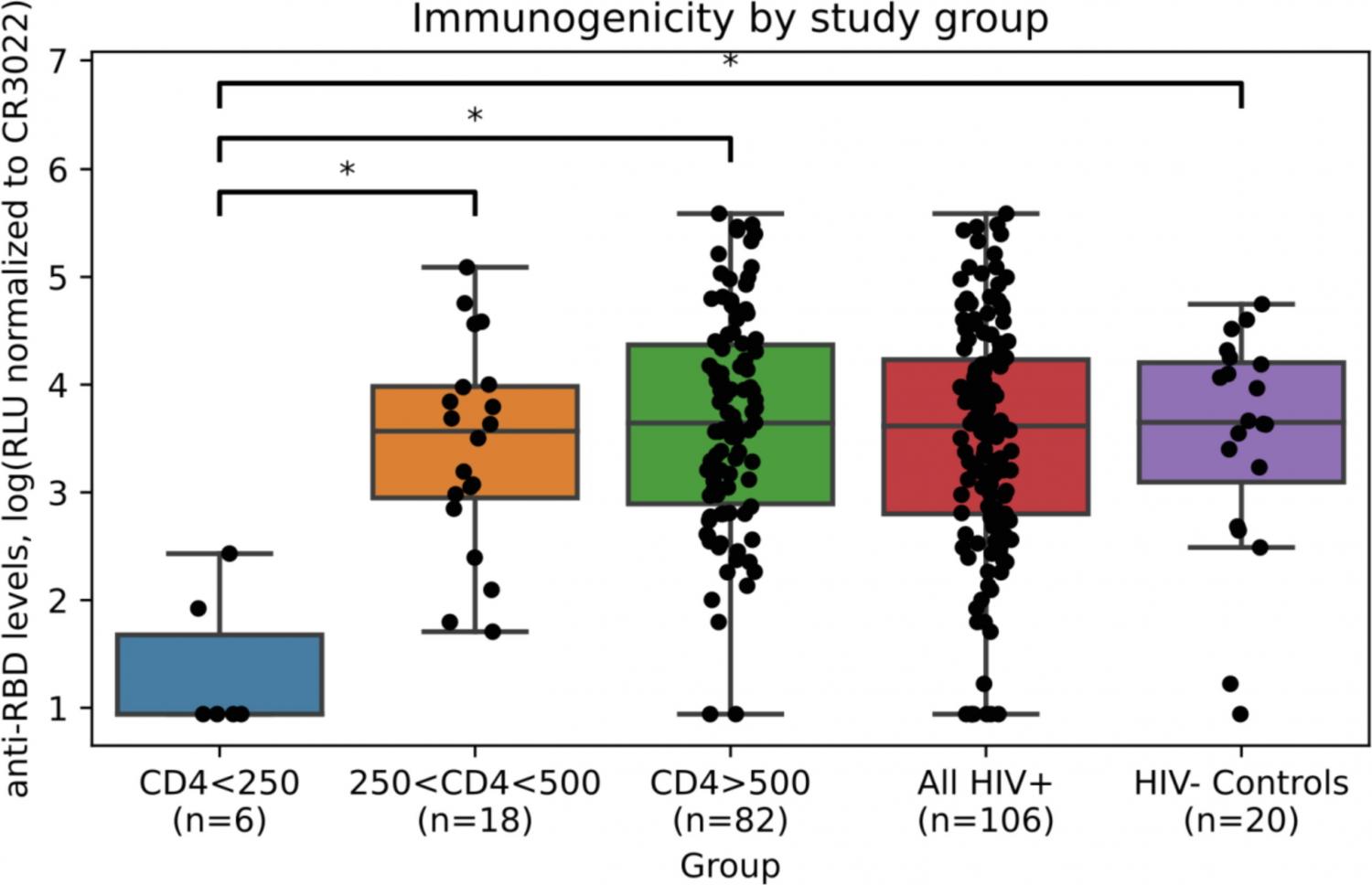
Introduction: COVID-19 vaccine efficacy has been evaluated in large clinical trials and in real-world situation. Although they have proven to be very effective in the general population, little is known about their efficacy in immunocompromised patients. HIV-infected individuals’ response to vaccine may vary according to the type of vaccine and their level of immunosuppression. We evaluated immunogenicity of an mRNA anti-SARS CoV-2 vaccine in HIV-positive individuals. Methods: HIV-positive individuals (n = 121) were recruited from HIV clinics in Montreal and stratified according to their CD4 counts. A control group of 20 health care workers naïve to SARS CoV-2 was used. The participants’ Anti-RBD IgG responses were measured by ELISA at baseline and 3–4 weeks after receiving the first dose of an mRNA vaccine). Results: Eleven of 121 participants had anti-COVID-19 antibodies at baseline, and a further 4 had incomplete data for the analysis. Mean anti-RBD IgG responses were similar between the HIV negative control group (n = 20) and the combined HIV+ group (n = 106) (p = 0.72). However, these responses were significantly lower in the group with <250 CD4 cells/mm3. (p < 0.0001). Increasing age was independently associated with decreased immunogenicity. Conclusion: HIV-positive individuals with CD4 counts over 250 cells/mm3 have an anti-RBD IgG response similar to the general population. However, HIV-positive individuals with the lowest CD4 counts (<250 cells/mm3) have a weaker response. These data would support the hypothesis that a booster dose might be needed in this subgroup of HIV-positive individuals, depending on their response to the second dose.